Documentation Index
Fetch the complete documentation index at: https://docs.pricemedic.com/llms.txt
Use this file to discover all available pages before exploring further.
Overview
The Provider Analysis dashboard allows you to benchmark your pricing against similar organizations in your region and specialty. Requirements for this dashboard include:- Access to Provider Profiles
Accessing the Dashboard
You can access this dashboard from your organization’s home screen by clicking the “Provider Analysis and Peer Comparison” card.Filters and Navigation

Navigation
The dashboard is organized into two primary sections:- Provider Overview: High-level insights and market positioning for your provider organization
- Competitor View: Detailed comparisons against specific competitor organizations in your market
Filtering Your Analysis
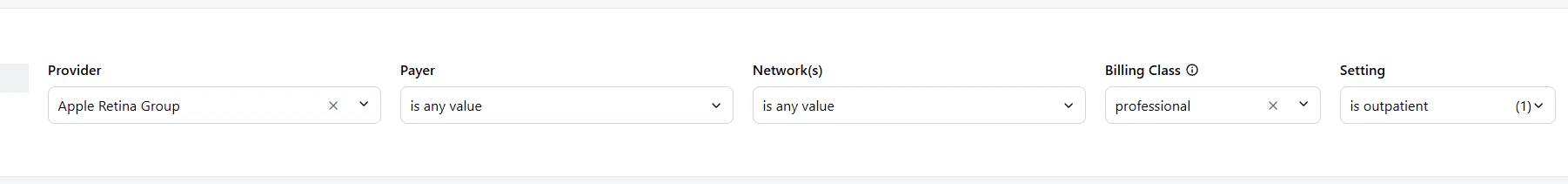
The filter bar at the top of the dashboard allows you to refine your analysis based on specific criteria. You can filter by provider, market, payer, network, billing class, and care setting. These filters apply across dashboard views in your session, allowing you to maintain a consistent analysis context as you navigate. Available Filters:- Provider: Select specific providers to analyze their pricing data.
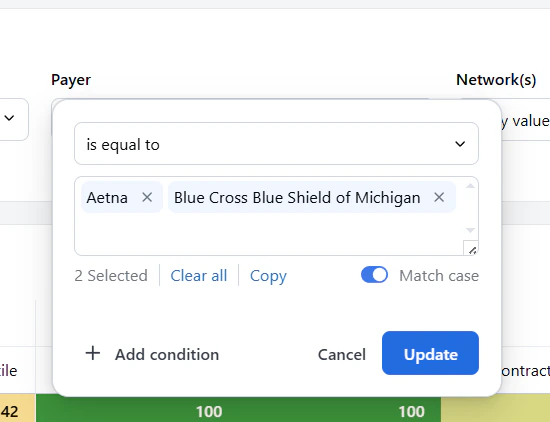
- Payer: Filter by specific insurance payers to see how your rates compare against them.
- Network: Filter by network type (e.g., in-network vs. out-of-network) to understand how your rates perform in different contexts.
- Billing Class: Filter by billing classification (e.g., professional vs. institutional) to analyze specific types of services.
- Setting: Filter by care setting (e.g., inpatient (facility) vs. outpatient (non-facility)) to see how your rates compare in different healthcare environments.
Exporting Your Data
You can export data from any table in the dashboard by clicking the three-dot menu in the top-right corner of the table and selecting “Download.” This lets you download the data in CSV format for further analysis or reporting.
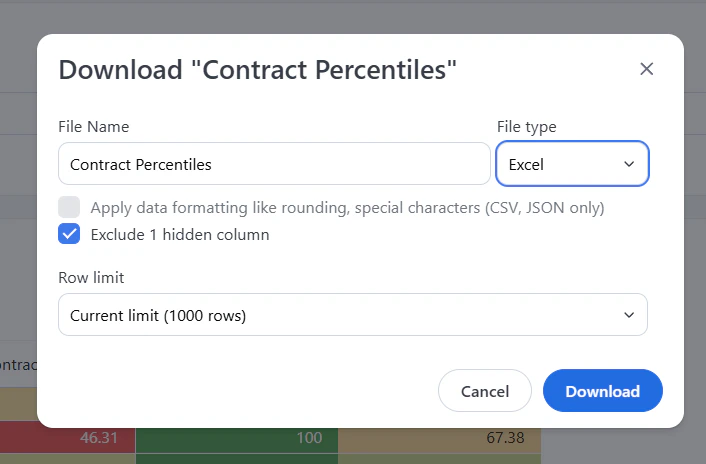
- Always select “Exclude hidden columns” if you have applied filters to ensure you only download the relevant data.
Dashboard Components
Contract Percentiles Table
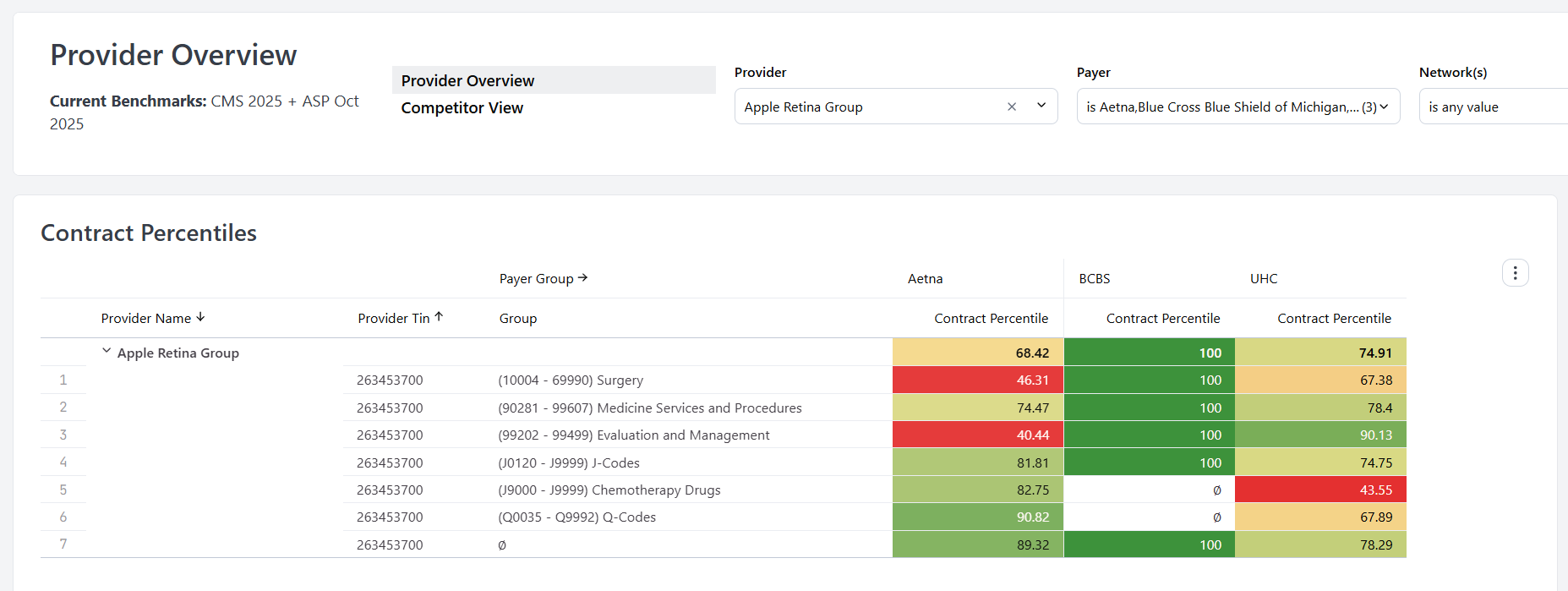
- BCBS (Blue Cross Blue Shield)
- Cigna
- Aetna
- UHC (UnitedHealthcare)
- Regional payers
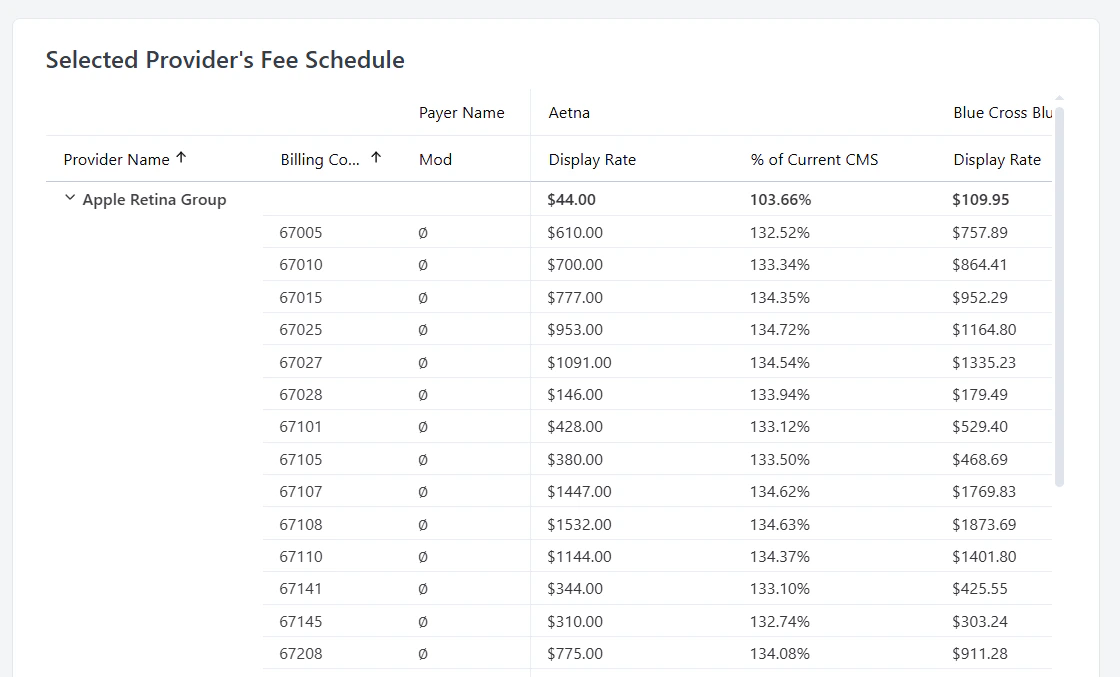
Selected Provider’s Fee Schedule
This table displays your provider’s current contracted rates for various payers. Each row represents a specific contract with detailed information including:- Payer Name: The insurance company name
- Billing Code: The specific CPT or procedure code
- Mod: Modifier codes that affect reimbursement
- % of Current CMS: Your rate expressed as a percentage of Medicare rates
- Display Rate: The actual dollar amount for the procedure
Market % of Medicare
A heat map visualization showing how different provider organizations compare to Medicare rates across the full distribution spectrum. The table displays percentiles ranging from the lower end of the market through the upper end, allowing you to see the complete picture of market pricing. Each row represents a different provider organization or claims group, with columns showing their reimbursement rates at different percentile levels expressed as percentages of Medicare rates. The heat map uses color gradients to quickly highlight performance patterns:- Red zones indicate rates below or near Medicare levels
- Yellow/neutral zones show moderate rates above Medicare
- Green zones highlight significantly higher reimbursement rates